[vc_row][vc_column][vc_column_text]
In Vitro Fertilization
In vitro fertilization (IVF) is the process of retrieving eggs and sperm and manually fertilizing them in a laboratory dish outside the woman’s body.
Once oocytes are fecundated, a limited number of obtained embryos are transferred into the woman’s womb, so they can continue developing in a natural way.
Procedure
IVF cycle has different stages:
- Study and preparation of the couple
- Ovarian stimulation
- Collection of oocytes
- Fertilization in laboratory: culture of oocytes, spermatozoa and embryos
- Transfer of embryos to the mother
IVF is generally used after having “blocked” the pharmacologically natural cycle and stimulated ovaries through a hormonal treatment to assure multiple follicular development.
Oocytes are taken out from the woman through an ultrasound-guided puncture and vaginal tube of the follicles. Immediately after they have been obtained they are prepared and classified in laboratory.
Sperm has to be obtained almost at the same time as extraction of oocytes, after a period of sexual abstinence. Sperm is prepared in the laboratory to remove certain components and to select the most adequate spermatozoa to fecundate the oocytes.
Spermatozoa are put in contact with oocytes, leaving them in incubation during certain hours.
Once fecundation is obtained, the best embryos are selected to be transferred to the woman’s womb.
The woman has to follow a hormonal treatment to help the feasibility of the potential pregnancy.

Intracytoplasmic Sperm Injection (ICSI)
ICSI is an intracytoplasmatic injection of spermatozoids into the oocyte.
When is it considered?
- Serious male factor
- Azoospermia (total absence of spermatozoa in ejaculate. Spermatozoa are obtained from testicular biopsy or epididymis aspiration)
- Oligozoospermia (low concentration of spermatozoa in ejaculate)
- Asthenozoospermia (pathological increase of spermatozoon mobility)
- Teratozoospermia (high percent of spermatozoa with abnormal morphology)
- Acrosomic anomalies
- Immunologic reasons. Antisperm antibodies
- “Valuable semen”. Patients who are going to have radio- or chemotherapy treatment, since although there is enough quantity to make an IVF or even an artificial insemination we would only dispose of a quantity for one or two cycles. With ICSI the possibilities will increase.
- Impossibility of taking the sample for psychological, ethical or paraplegic reasons, or nervous section that prevents ejaculate.
- Failure in IVF fecundation. Or low fertilization ratio or high polyploidy rates.
- Failure of artificial insemination. If we microinject at least half of the oocytes obtained from patients with three AI failures in the first cycle of IVF we guarantee as a minimum transfer of embryos.
- PGD (Preimplantation Genetic Diagnosis): When running a PGD, ICSI is more recommended than IVF, since the latter might bring some contamination with spermatozoa, distorting the results.
Procedure
This procedure is almost identical to in vitro fecundation. The only difference is the handling of the obtained oocytes after the puncture, since they undergo a more labored micromanipulation technique than a conventional IVF.
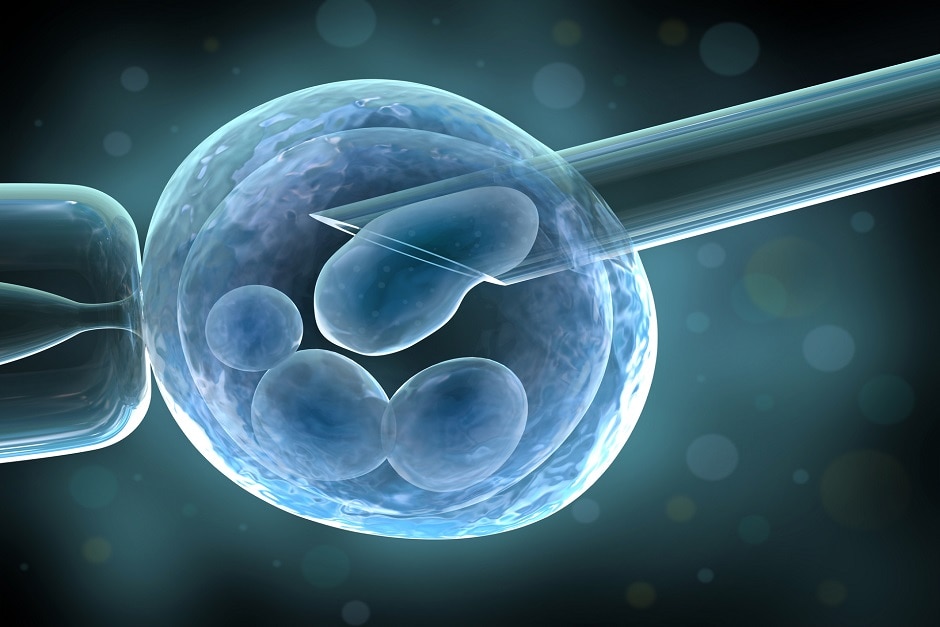
Vitrification
Since 2005, Aisa Reproduction in Spain, has been implementing a new method of cryopreservation: Vitrification, (commonly known as Flash Freezing). It avoids the damage of the cell by ice crystal formation and other effects seen with slow freezing.
According to latest studies published, it has been proved that pregnancies obtained through vitrification are more similar to the natural conception than pregnancies with fresh embryos.
This results into an increase in pregnancy rates and pregnancy evolution, higher live birth rates, lower miscarriages and lower risk of premature birth.
Embryos are frozen by means of this technique after an ovaric stimulation cycle. Then we wait to the next natural cycle of the patient to transfer the thawed embryos to the patient, bringing hormonal levels down to normal. This process is much more alike to a natural pregnancy.
Besides, by not transferring the embryos right after an ovaric stimulation, we decrease enormously the risk of ovaric hyper stimulation derived from the medication needed to obtain oocytes, which is one of the most relevant side effects this medication has.
In Aisa Reproduccion, we achieved the first birth with vitrification in 2005.
Our survival rate of embryos and oocytes in any stage is 100%.

Chromosome Screening (CS)
Aisa Reproduction in Spain, has been using this technique since 2012.
It allows analyzing genetically the embryos before being transferred to the womb. Thus, we select only the embryos without genetic abnormalities.
Around 50% of embryos from women of 38 years old carry some kind of genetic abnormality, leading to high rates of early miscarriage.
The Array-CGH is a specific chromosome screening technique based on Compared Genomic Hybridization, which allows to analyze the full genomic sequence of the embryo in just one test, looking for alterations in gain or loss of genetic material.
Opposed to the 9 pairs of chromosomes traditionally analyze with FISH techniques, the Array-CGH analyses the full 23 pairs of chromosomes.
The test is performed through a biopsy to a day 3 embryo that has between 6 and 8 cells. We extract one of those cells to be analyzed. The embryo and the genetic material are not altered in any way during the process. While awaiting the results, we let the embryo grow for two more days, until it becomes a blastocyst.
This test is fast and very reliable. We can provide you with the results in less than 48 hours.
Women should consider a Chromosome Screening when they:
- Are 35 years of age or older.
- Have a history of repeated miscarriage.
- Had a previous pregnancy involving chromosomal abnormality
- Had several IVF failures
- Had translocations
The Chromosome Screening brings the highest rates of babies born with assisted reproductive techniques.
The combination of Vitrification and Chromosome Screening has relevant benefits for the patient, enhancing the likelihood of implantation and healthier pregnancy and birth.
Preimplantation Genetic Diagnosis (PGD)
The Preimplantation Genetic Diagnosis (PGD) enables to analyze the embryos before transferring them into the womb. Thus, selecting only the embryos without genetic anomalies. PGD is a new technique that helps the achievement of health pregnancies using In Vitro Fertilization.
There are two types of patients that should be usually opting for this technique:
- A member of the couple, or both, are carrying a serious genetic disease and would like to prevent its transmission to their descendants.In this case, the first step is to go through a full genetic reproductive consultation, in which all topics are addressed and questions answered to the patients.A genetic study follows, in which the family DNA is analysed so we can obtain the adequate diagnosis to be run with the embryos.Once this study is done, we can start with the IVF process. Once we have obtained the oocytes and fertilized them in our laboratory, the embryos are kept during three days so they are mature enough for an embryonic biopsy.The results of the biopsy are available within 48 hours. During that period, the embryos are kept in the laboratory maturing to blastocyst stage.The PDG is allowed by law and recommended for any serious genetic disease (Law 14/2006, de 26 de mayo, sobre técnicas de reproducción humana asistida, art.12.1.a y 12.2).
- The second type of patients doesn’t have any serious genetic disease. However, they have unsuccessfully tried several IVF cycles. This may indicate the existence of genetic alterations in the embryo. Therefore, what is called a genetic diagnosis for aneuploidy screening (GDAS) is highly recommended in the following cases:
- Repeated miscarriage
- Implantation failure
- Advance age of the patient (A 38-year-old woman can have 50% of embryos with genetic anomalies) Running a PGD would enable not to transfer those embryos.
- Severe male infertility factor
We use a technique called ARRAY-CCH, which is based on Comparative Genomic Hybridization, allowing analyzing all the genome sequence, looking for genetic alterations.
This process is fast and very reliable, being able to have full results in less than 48 hours. Other techniques, such as FISH, allow analyzing 9 pairs of chromosomes.
ARRAY analyzes the full 23 pairs of chromosomes.
The PGD brings the highest rates of “healthy child at home” using IVF techniques.

Intrauterine Insemination (IUI)
Intrauterine Insemination (or artificial insemination) is the introduction of semen, previously qualified in the laboratory, into the uterine cavity some hours before ovulation.
When to consider intrauterine insemination?
- Ovulation disturbance
- Decreasing number or mobility of spermatozoa, and/or anomalies in these
- Difficulty in penetration of spermatozoa in the uterine cavity
- Infertility or sterility for unknown reason
- Others
Procedure
Intrauterine insemination can be carried out during the natural cycle, or after an ovarian stimulation process. It has been demonstrated, in a large number of studies, that rate of pregnancy is significantly higher in those cycles in which ovulation has been stimulated.
Ovulation stimulation consists of a hormonal treatment carried out by administrating a series of drugs, given to assure the ovulation and to obtain the highest number of oocytes.
To control it, periodical ultrasound tests are made, sometimes along with blood analysis, to verify the increase of the follicles and hormonal levels, in order to decide the best moment for insemination.
On the day of insemination, the male has to come with a sample of semen, which is processed in the laboratory, by an adequate preparation, selecting spermatozoa with best mobility.
Afterwards, spermatozoa are introduced in uterine through a flexible catheter.
Once insemination is done the women starts a hormonal treatment that favors the development of the possible gestation.
Models
There are three models of intrauterine insemination:
- With semen from donation (AID)
- With semen from husband/couple (AIH)
- Artificial insemination with semen from husband with a negative PCR determination in inseminated sperm (AIH-HIV), so transmission of the disease to partner and offspring is avoided (in case she doesn’t suffer from it).
Donor Program
Egg Donor Program
Our Egg Donor Program can bring families the possibility of successful pregnancies when:
- There is an ovarian failure
- Low quality of own eggs
- Women in an old reproductive stage
- Chromosomal translocations or genetic diseases
It is an anonymous procedure in which donor gives oocytes to beneficiary woman.
Our staff rigorously screens egg donor candidates to ensure they are healthy and that they fully understand the donation process. Our egg donor pool consists of donors from a variety of racial and ethnic backgrounds. The donor must go through the following testing procedures before being accepted:
- Be of legal age (between 18-35)
- Medical history and physical examination
- Testing for infectious diseases
- Hereditary transmitted diseases and chromosome analysis
- Screening for inheritable diseases through family health questionnaire
There is no waiting list in our Donor Program
While egg quality deteriorates with age, a woman’s uterus and her ability to carry and deliver a child remains relatively constant. Therefore, egg donation offers a substantially higher chance for the delivery of a healthy baby, even in women of advanced maternal age.
Our success pregnancy rates are above 75%.
Sperm Donor Program
Donors have to fulfill certain requirements (non-carriers of genetic, hereditary or sexually transmitted diseases, be a person legally of age, have a normal intelligence coefficient, etc.) and their sperm has to match the quality required by our Centre.
In addition they must sign a document, which allows us to use their sperm in assisted reproductive techniques so as to assume the same inherent anonymity.
Sperm is preserved frozen from its taking until the moment of its use, staying in this state for a minimum of six months to verify no contagious risk of sexually transmitted diseases.
Donor’s characteristics are chosen in accordance with phenotype of beneficiary patients.
Do you want to become a donor?
You can help many others to have (or expand) their own family

[devider size=”full” thickness=”2px” ]
Fertility Preservation
If you have the desire to postpone building a family – for a multitude of reasons. For example, in the case of age and not ready yet to start a family, you have a low ovarian reserve or poor responder reserve, or if you are older and you wish to bank embryos for attempting later pregnancies, we offer you the possibility of doing so.
By retrieving your eggs and flash-freezing them through our vitrification technique, which guarantees a 100% survival rate of oocytes or embryos.
The oocytes, or embryos, in case you decided to undergo an IVF cycle, will then be stored frozen in our bank until you are ready to be a mother.
Considered for all kind of women: for young women who want to preserve their fertility due to career choices. Or women who have been diagnosed with cancer and must go through chemotherapy.

Single Parents
Aisa Reproduction in Spain, supports any individual in her or his aim of having a family.
We have a Sperm Bank with donors from different ethnics and phenotypes.
Once we have selected the anonymous donor, the sperm can be used in any of the fertility treatments that you and our physicians may consider to your case (IVF, ICSI, IUI…)

Same-Sex Parents
At Aisa Reproduction in Spain, we support all types of family building within law and therefore we provide patients with the necessary means to make their dreams come true. We collaborate with the Lesbian and Gay community to continuously understand their needs and to provide them with the best available treatment and emotional care.
We keep an Egg Bank, as well as a Sperm Bank, as part of our Donor Program.
 [/vc_column_text][/vc_column][/vc_row]
[/vc_column_text][/vc_column][/vc_row]